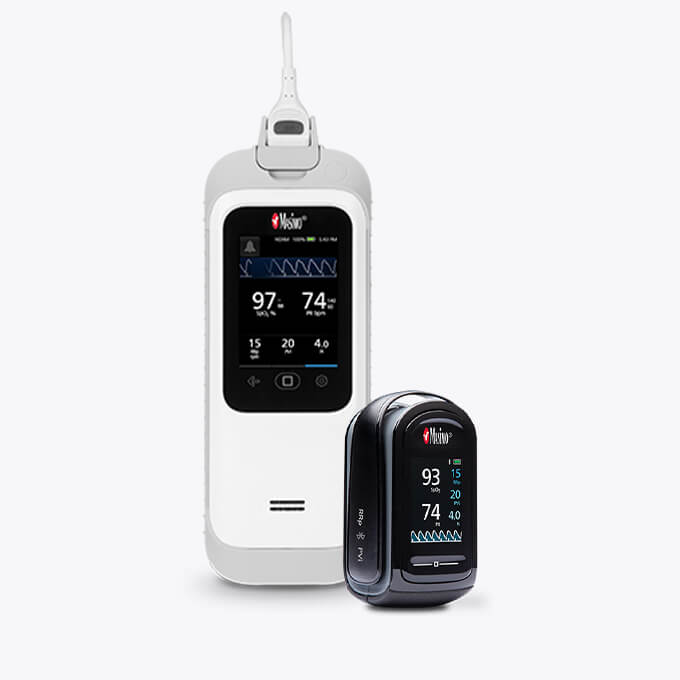
Pulse Oximeters
A pulse oximeter is a small, non-invasive device that clips onto a finger, toe, or earlobe to measure blood oxygen saturation (SpO2) and pulse rate. It uses red and infrared light sensors to assess how much oxygen your blood is carrying, delivering readings within seconds for clinical observation and home monitoring.
More Information
Pulse Oximeters UK Pulse oximeters are used across primary care and home settings amongst others to monitor oxygen saturation and heart rate in real time. They support early detection of hypoxia, assist in respiratory condition management, and provide valuable trend data during acute illness or recovery. Common clinical uses include: • Monitoring chronic respiratory conditions such as COPD and asthma • Observing patients with suspected or confirmed long COVID • Assessing respiratory status during infection or acute illness • Monitoring the effects of opioids, sedatives, or anaesthesia • Routine inpatient and outpatient observations • Home self-monitoring for high-risk or clinically vulnerable individuals By enabling quick, non-invasive measurement without the need for blood sampling, pulse oximeters support earlier intervention and informed clinical decision-making. How Pulse Oximeters Work Pulse oximeters estimate arterial oxygen saturation (SpO2) using photoplethysmography. The device emits red light at approximately 660 nm and infrared light at approximately 940 nm through tissue. Oxygenated and deoxygenated haemoglobin absorb these wavelengths differently. By analysing these absorption patterns and calculating a “ratio of ratios,” the device estimates oxygen saturation and displays pulse rate. Modern clinical-grade devices are highly accurate in healthy adults, typically within 2 to 3 percent of arterial blood gas measurements. However, readings should always be interpreted in the context of the patient’s overall clinical presentation. When to Use a Pulse Oximeter Illness Monitoring Pulse oximetry is widely used in the management of chronic lung disease. COPD affects approximately 12 percent of UK adults over 65. Long COVID continues to affect around 1.9 million UK residents according to recent ONS data. In these populations, monitoring oxygen saturation helps identify deterioration early and supports safe community-based care. Medication and Post-Operative Monitoring Respiratory depression can occur with opioids and sedatives. Post-operative desaturation has been observed in approximately 20 percent of surgical patients, making pulse oximetry a valuable monitoring tool in recovery settings. Routine Clinical Observations Pulse oximeters form part of routine observation protocols in hospital wards, urgent care, GP practices, and community healthcare settings. Trending oxygen saturation over time can provide early warning of clinical deterioration. Home Monitoring For selected high-risk patients, home pulse oximetry enables structured monitoring plans agreed with clinicians. Clear escalation guidance should always accompany home use. Normal Readings and When to Escalate For healthy adults, normal oxygen saturation is typically between 95 and 100 percent. Normal resting pulse rate ranges from 60 to 100 beats per minute. Patients with chronic lung disease may have a lower clinically agreed baseline, often between 88 and 92 percent, as determined by their healthcare provider. Escalation guidance: • Below 94 percent at rest: repeat measurement and assess symptoms • Persistently below 92 percent: or associated with breathlessness, confusion, or cyanosis: contact GP or NHS 111 • Below 88 percent or severe symptoms: call 999 immediately Pulse oximeters should never be used in isolation. Clinical symptoms and professional judgement remain essential. Benefits of Pulse Oximetry • Non-invasive and painless • Rapid results within seconds • Portable and suitable for point-of-care use • Supports early detection of hypoxia • Enables monitoring without repeated blood sampling Clinical trials in COPD populations have shown that structured oxygen monitoring programmes may reduce hospital admissions by 20 to 30 percent when combined with clear care pathways. Accuracy, Limitations, and Clinical Considerations While pulse oximeters are highly useful, several factors can affect accuracy. Skin Tone Evidence reviewed in recent FDA guidance indicates that some devices may overestimate oxygen saturation by approximately 1 to 2 percent in individuals with darker skin tones. This does not render devices unsafe, but clinicians should interpret readings alongside symptoms and consider repeat assessment where clinical suspicion remains high. Nail Polish and Artificial Nails Dark nail polish or artificial nails may interfere with light transmission and introduce errors of up to 3 percent. Removal prior to testing is recommended where possible. Poor Peripheral Perfusion Cold extremities, hypotension, or poor circulation may increase measurement variability. Warming hands and ensuring adequate perfusion can improve reliability. Movement and Ambient Light Excessive motion or strong external light sources may disrupt signal stability. Patients should remain still during measurement. Low Saturation Levels Pulse oximeters become less accurate at very low oxygen levels. Below 70 percent SpO2, accuracy decreases significantly because the device struggles to differentiate light absorption patterns at extreme desaturation levels. In critical care settings, arterial blood gas analysis remains the gold standard. Hidden Hypoxaemia Rarely, patients may have lower arterial oxygen levels than pulse oximetry suggests. This reinforces the importance of clinical assessment and not relying solely on device readings. Pulse oximetry is a supportive tool. It does not replace clinical examination or diagnostic testing. How to Use a Finger Pulse Oximeter 1. Allow the patient to rest for at least five minutes. 2. Ensure hands are warm and relaxed. 3. Remove nail polish or artificial nails if possible. 4. Place the device on the middle or index finger with the nail facing upward. 5. Keep the hand at heart level and remain still. 6. Wait 30 to 60 seconds for a stable reading. 7. Record results and monitor trends where appropriate. 8. Clean the device according to manufacturer guidance after use. Trend monitoring is often more clinically useful than a single isolated reading. Our Range at Williams Medical Supplies At Williams Medical Supplies, we stock CE-marked, ISO 13485-certified fingertip and handheld pulse oximeters from leading manufacturers including Mesi, Nonin, and Masimo. Our range supports use across primary care, hospital environments, and community settings. Prices start from £38.99 ex VAT, with free delivery available on orders over £100. Our team is available to advise on device selection based on clinical setting and patient population. For blue light and emergency service teams operating in pre-hospital and high-acuity settings, explore the SP Services range of pulse oximeters, selected specifically for demanding frontline environments. Looking for pulse oximeters for home use? View eSupplies Medical range of fingertip pulse oximeters for home testing. Pulse Oximeter Frequently Asked Questions What do pulse oximeters measure? A pulse oximeter measures blood oxygen saturation, known as SpO2, and pulse rate. SpO2 indicates the percentage of haemoglobin in the blood that is carrying oxygen. The device provides a quick, non-invasive estimate of oxygen levels by using light sensors placed on the finger, toe, or earlobe. It is commonly used in hospitals, GP practices, and home settings to support respiratory monitoring and early detection of hypoxia. What does a pulse oximeter measure besides oxygen levels? In addition to oxygen saturation (SpO2), a pulse oximeter measures pulse rate in beats per minute. Some advanced models may also display pulse waveform or perfusion index, which can indicate signal strength and circulation quality. However, pulse oximeters do not measure breathing rate, lung function, or blood pressure. They are designed specifically to estimate oxygen levels and heart rate. Can a pulse oximeter measure blood pressure? No, a pulse oximeter cannot measure blood pressure. It estimates oxygen saturation and pulse rate using light-based sensors. Blood pressure requires a separate device, such as a manual sphygmomanometer or digital blood pressure monitor. While pulse rate is related to cardiovascular function, it does not provide information about systolic or diastolic blood pressure levels. Which finger is best for a pulse oximeter reading? The middle or index finger of either hand is typically recommended for accurate pulse oximeter readings. The device should be placed with the nail facing upward, and the hand should be warm and relaxed. Cold fingers, poor circulation, or movement can affect accuracy. Consistency is important, so using the same finger for repeat measurements can help track trends more reliably. What conditions can cause a false pulse oximeter reading? False or inaccurate readings can occur due to cold hands, poor circulation, movement, nail polish, artificial nails, or strong ambient light. Some studies also indicate that certain devices may slightly overestimate oxygen levels in individuals with darker skin tones. Severe anaemia or very low oxygen levels can also affect reliability. Readings should always be interpreted alongside symptoms and clinical assessment. How accurate are pulse oximeters in adults and children? Clinical-grade pulse oximeters are generally accurate within 2 to 3 percent of arterial blood gas measurements in healthy adults. Accuracy may vary slightly in children, particularly infants, due to movement or smaller finger size. Paediatric-specific pulse oximeter sensors improve reliability. Readings are most dependable when the patient is still, warm, and well-perfused. Pulse oximetry supports assessment but does not replace clinical judgement. What is a normal oxygen level on a pulse oximeter? For healthy adults, a normal oxygen saturation level typically ranges between 95 and 100 percent. Pulse rate usually falls between 60 and 100 beats per minute at rest. Values may vary slightly depending on age, altitude, and overall health. Readings should be considered in context, particularly if symptoms such as breathlessness or chest discomfort are present. What is a good SpO2 level for elderly adults? In most elderly adults, a good SpO2 level remains between 95 and 100 percent. However, individuals with chronic lung conditions such as COPD may have a clinically agreed baseline between 88 and 92 percent. Oxygen targets should always follow medical guidance specific to the patient. Any persistent drop below a person’s normal baseline should be assessed by a healthcare professional. What is a normal oxygen level while sleeping? Oxygen saturation may decrease slightly during sleep, but in healthy individuals it typically remains above 94 percent. Brief dips can occur, particularly during deep sleep. Persistent levels below 90 to 92 percent during sleep may require medical evaluation, especially if accompanied by snoring, pauses in breathing, or daytime fatigue, which could indicate sleep-disordered breathing. What is a normal oxygen level for a child? In healthy children, normal oxygen saturation is usually between 95 and 100 percent, similar to adults. In infants and young children, movement can affect readings, so ensuring proper sensor placement and minimal motion is important. Paediatric pulse oximeters or appropriately sized probes are recommended for smaller fingers to improve accuracy and comfort during monitoring. What is a dangerously low oxygen level on an oximeter? An oxygen saturation level below 92 percent is generally considered concerning and should prompt medical advice, particularly if symptoms are present. Levels below 88 percent are typically regarded as a medical emergency. Severe breathlessness, confusion, chest pain, or bluish lips alongside low readings require urgent assessment. Clinical context and symptoms are always essential when interpreting results. What are the signs that someone needs oxygen? Signs that someone may need oxygen include persistent shortness of breath, rapid breathing, chest discomfort, confusion, extreme fatigue, or bluish lips and fingertips. A pulse oximeter reading below normal levels may support these findings, but symptoms are equally important. Anyone experiencing severe breathing difficulty or sudden deterioration should seek urgent medical attention immediately. What is silent hypoxia? Silent hypoxia refers to a condition where blood oxygen levels are low without obvious symptoms of breathlessness. Individuals may feel relatively comfortable despite dangerously low oxygen saturation. This phenomenon gained attention during COVID-19, where patients sometimes presented with severe hypoxia but minimal distress. Pulse oximetry can help detect silent hypoxia, but clinical assessment remains essential. What is the most common cause of low blood oxygen? The most common causes of low blood oxygen include respiratory infections, chronic lung diseases such as COPD or asthma, pneumonia, and heart conditions affecting oxygen circulation. Acute illnesses that impair lung function can also reduce oxygen levels. Identifying and treating the underlying cause is critical, as pulse oximeters measure oxygen levels but do not diagnose the reason for desaturation. Do adult pulse oximeters work on children? Some adult fingertip pulse oximeters may work on older children if the finger fits securely within the sensor. However, they may not provide reliable readings in infants or very young children due to smaller finger size and movement. Paediatric-specific devices or probes are recommended in clinical settings to ensure accurate, stable measurements and appropriate comfort. Disclaimer: This information is provided for educational purposes only and does not replace professional clinical judgement. Pulse oximeters are not diagnostic devices and should always be interpreted alongside patient symptoms and assessment findings. If readings are low or symptoms are concerning, urgent medical advice should be sought in line with NHS guidance.